Patients with non-metastatic stomach or gastroesophageal junction cancer usually receive a combination of radiotherapy and chemotherapy before their surgery, or chemotherapy both before and after their surgery. Despite advances in treatment of this cancer type, the prognosis has not shown improvement. Researchers looking to improve the prognosis for these patients have conducted a phase-2 PANDA trial, focusing on a new treatment type. They investigated the effects of the combination of immunotherapy and chemotherapy before surgery. This treatment showed a significant tumor reduction in a large number of patients.
In the trial, 20 patients with this cancer type received this combination therapy. They started with one course of immunotherapy drug atezolizumab, followed by four courses of atezolizumab while receiving chemotherapy. 14 out of 20 patients responded well to the treatment—in 9 patients, the tumor even disappeared entirely. Nearly four years after treatment, most patients with reduced tumors were still cancer-free. Furthermore, the patients tolerated treatment well, mainly experiencing mild side effects. Only a small percentage experienced side effects that were more severe.
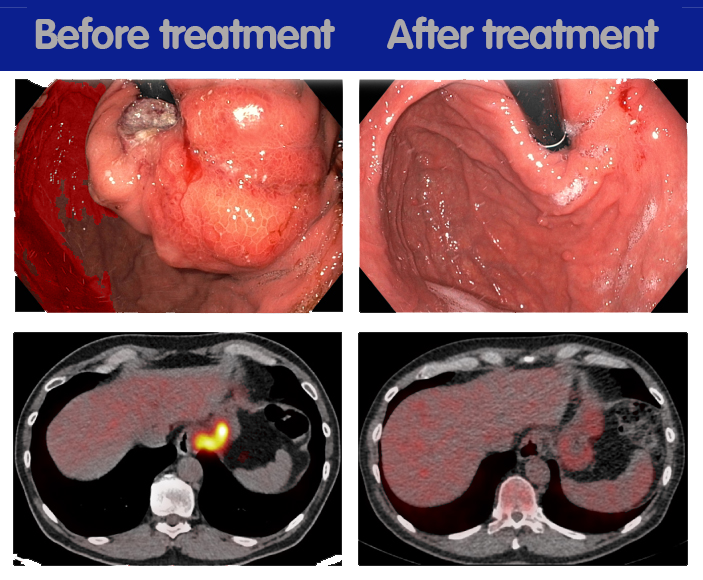
"The trial shows promising results, indicating that this treatment is effective for patients with stomach or gastroesophageal junction cancer. This combination of immunotherapy with chemotherapy seems promising and may open up new possibilities to treat these complex cancer types," says medical oncologist and researcher leader Myriam Chalabi. One thing that makes this trial unique, she adds, is that patients received their first course of immunotherapy without simultaneously receiving chemotherapy, which appears to lead to better results than similar studies into the combination of chemotherapy and immunotherapy.
The researchers also discovered that certain immune cells in the tumor area were very active after the first course of immunotherapy in the patients who responded well to the treatment. This suggests a positive link between the immune response and the effects of the treatment and could be a way to predict whether it will be effective at a very early stage. Medical researcher Yara Verschoor: “We also found that the presence of certain immune cells before the start of treatment may potentially help us predict effectiveness. If we see this same result in larger studies, we may be able to better select patients who benefit from this treatment.”
Despite its small scale, the results of this trial are promising and suggest that this approach should be further investigated in larger groups of patients. It offers new hope for a more effective treatment for patients with stomach and esophageal cancer in the future.